Clarington Physiotherapy Health and Wellness Centre Blog
Vestibular Rehabilitation Therapy? What’s that?
Our physiotherapist Jezreel Suyom is launching a Vestibular Rehabilitation Therapy at the clinic, which we are really excited about! Jez is now a certified vestibular physiotherapist after completing his…
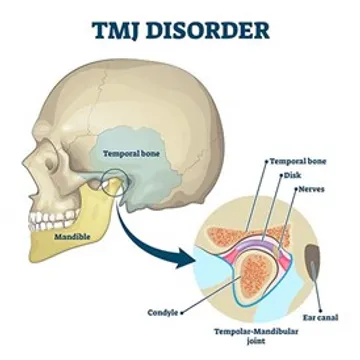
What is the TMJ and how can we treat it?
You may have heard of a TMJ injury in the past; however, you may not know exactly what that means. TMJ stands for temporo-mandibular joint, or the jaw joint…
Pelvic Pain Awareness Month
Chronic pelvic pain (CPP) negatively affects millions of people across the gender identity spectrum throughout the world (International Pelvic Pain Society, IPPS). It can impact a person’s physical, emotional, and…
Do you have Texting thumb?
A large group of us have been spending more time scrolling through the news on our phones and our social media posts these days. This repetitive motion can create…
Do you suffer from constant headaches?
Headaches: not only are they painful, but they can also be disabling. Did you know that headaches are among the most common disorders of the nervous system?There are many…
The Total Pain Education Package (Part 2)
I’m going to continue on with the pain education I started in my last post (see https://www.claringtonphysio.ca/post/the-total-pain-education-package-part-1 for part 1). As always, remember pain can be complicated, and if…
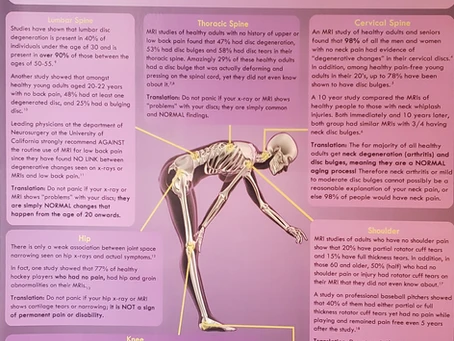
The Total Pain Education Package (Part 1)
What is “PAIN”? It’s something we all experience, something that in general we don’t like, and yet most of us know very little about it. I decided to put…
What have we been up to during quarantine?
Hello! Hope you and your families have been well and have been safe during this pandemic season. Hope you’ve found some new hobbies and projects to keep you busy…
Spring running season is here!
Running is a great way to get some fresh air and exercise, as long as you still maintain social distancing! Although running is a great method of exercise, it…